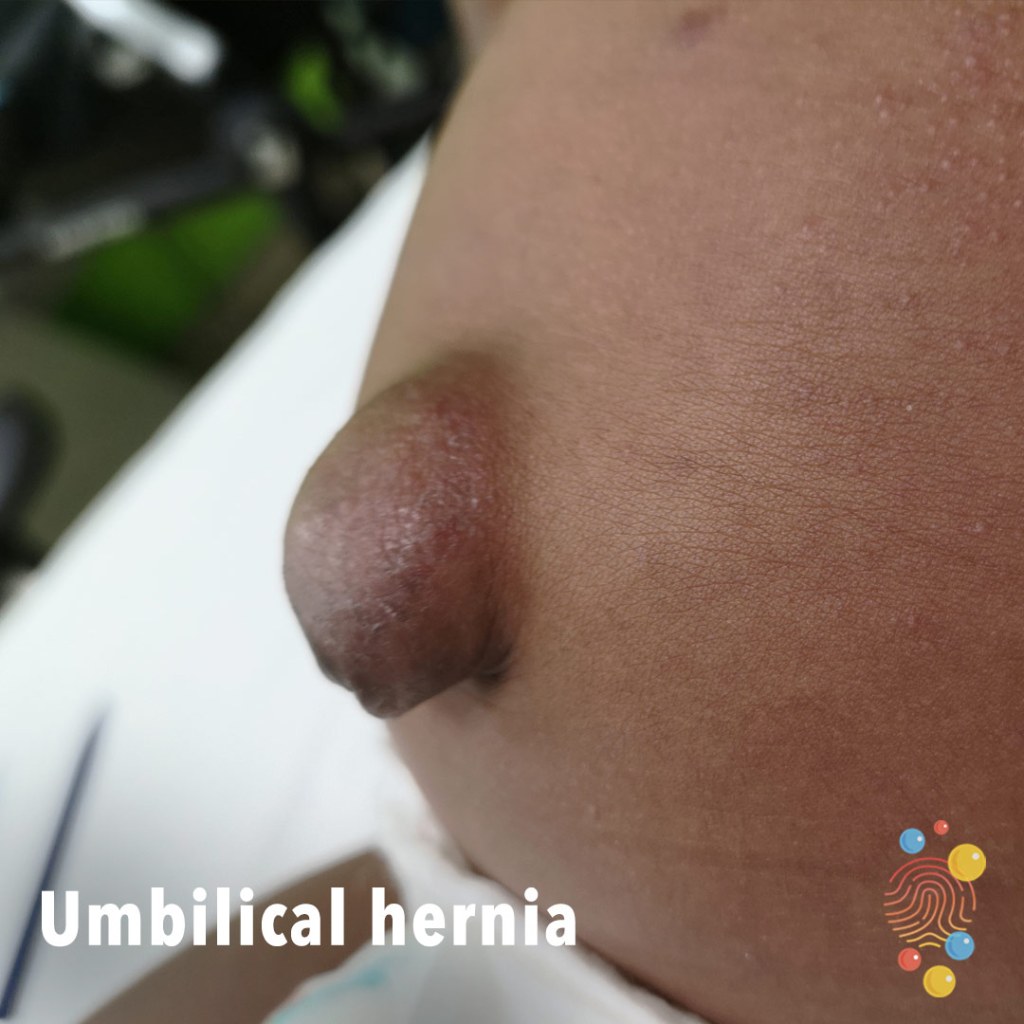
What are hernias?
Hernias occur when fatty tissue or organ tissue, such as the bowel, bulges through a weak area in the surrounding fascia or muscle. Various hernias can present in children. These include umbilical, epigastric, inguinal and femoral hernias. Some are more common than others. Being able to differentiate between them can help you determine the urgency of treatment.
Types of hernias
Umbilical hernias
These hernias usually present as a painless, reducible bulge at the umbilicus. They become more evident as intra-abdominal pressure increases with straining or crying. These hernias are more common within the African population, but the reason behind this is unknown.
Epigastric hernias
Epigastric hernias are seen along the midline, between the xiphoid process and the umbilicus. They mostly contain preperitoneal fat. Children normally present with a mass in the epigastrium. This mass can get bigger and may be associated with abdominal wall tenderness or pain. The hernia may rub against clothing, leading to more pain and skin irritation. Approximately 10% of epigastric hernias present as multiple defects, resulting in multiple midline lumps.
Inguinal hernias
Inguinal hernias normally present as a bulge in the groin that can be seen or is exacerbated when the child is crying or straining. It could also be a swelling in the scrotum. In boys, it is important to consider the range of possible differential diagnoses for a groin lump, such as hydrocele, undescended testes, and varicocele.
Inguinal hernia vs hydrocele
One method used to differentiate inguinal hernias from hydrocele is transillumination; however, this method should be used with caution, as both inguinal hernias and hydroceles can transilluminate in very young patients (particularly neonates).
A more exact method involves palpating the lump. You can get above a hydrocele, which isn’t possible in a hernia due to the continuous patent processus vaginalis. Alternatively, you can feel for the ‘silk glove sign’: rolling the cord structures against the pubic tubercle with an index finger feels like two silk sheets rubbing against one another if it’s an inguinal hernia. What you are feeling is the smooth edges of the peritoneal sac. The safest approach, however, is an ultrasound scan if you’re in doubt!
Lateral to pubic tubercle, they become more evident with raised intraabdominal pressure (i.e. crying, coughing, sneezing).

Female inguinal hernias
Inguinal hernias don’t just occur in boys. They also occur in girls, and ovaries can become trapped. The ovary feels firmer to touch and maybe more mobile, whereas the bowel tends to feel more squishy. A unilateral, erythematous, swollen labia can result from a torted ovary that has passed through the patent processus vaginalis.
Femoral hernias
These are extremely uncommon in children (and account for less than 1% of groin hernias in children) and present as a bulge lateral to the pubic tubercle. They can be mistaken for inguinal hernias but may present as a reducible recurrent groin lump. They tend to occur on the right side.
Why do hernias occur?
There is no definitive causative factor for hernias in children. It is thought that umbilical hernias may be related to the delayed closure of the umbilical cord ring through which the umbilical vessels between mother and fetus used to pass.
Epigastric hernias might result from incomplete joining of the upper abdominal wall muscles (linea alba), which allows fatty tissue to push through.
Paediatric inguinal hernias are caused by a persisting patent processus vaginalis. This structure allows for the migration of the testis from the posterior abdominal wall, through the inguinal canal, into the scrotum during the 3rd to 7th month in utero. Hence, abdominal contents can herniate through the deep inguinal ring, inguinal canal, superficial inguinal ring, and into the scrotum or through the canal of Nuck into the labia.
Assessing the hernia
Always take a thorough history and examination. Sometimes, hernias can appear secondary to the primary condition, causing a child to cry or become distressed.
It is also important to differentiate an epigastric hernia from a divarification of the recti. Divarification occurs when there is a weakness in the linea alba, which can result in a uniform bulge that runs down the midline from the xiphoid process to the umbilicus. This isn’t a hernia and will resolve as the child grows and muscle tone develops.
There’s a 5-20% probability of an inguinal hernia developing bilaterally, so check both sides. After repair of one side, another one can develop on the contralateral side. An incarcerated inguinal hernia may become irreducible, and the majority of these occur in infants.
It is important to differentiate between an inguinal hernia and other inguinoscrotal masses as the cause helps determine the urgency of treatment. Inguinal hernias may be confused with a communicating hydrocele, a benign condition. For the most part, hernias and hydroceles are repaired similarly; however, hydroceles pose a smaller health risk and are thus less urgent. They may even spontaneously resolve over time).
Red flags
Never disregard a bulge or lump in an infant if they are distressed or in pain.
Pain suggests incarceration and imminent strangulation of the hernia content (e.g. bowel).
Incarceration occurs when the viscera or omentum becomes stuck within the hernia. It presents as a painful, irreducible lump that may change colour. Children might complain of pain or tenderness.
Strangulation occurs when the blood supply to the viscera is compromised. This results in ischaemia, tissue damage and necrosis. Strangulation can cause children to vomit, become constipated, become feverish, or have blood in their stool.
Management of hernias
If incarceration or strangulation is suspected, urgent assessment by the paediatric or general surgical team is needed.
Umbilical hernias
Umbilical hernias are commonly seen during the newborn exam. No treatment is usually required as these hernias tend to resolve by 3 years of age. If the hernia is no longer reducible, this is a cause for concern and should be referred.
Parents may be quite anxious and worried about the lump and its appearance when their child is unwell or distressed, so it’s important to reassure them that asymptomatic reducible umbilical hernias rarely result in complications and mostly close spontaneously by the time the child is four years old. If the hernia hasn’t closed by age 4, it would be appropriate to refer them to the paediatric team/surgeon, as spontaneous closure is less likely to occur as the child grows.
Epigastric hernias
Two-thirds of epigastric hernias are reducible and asymptomatic; however, they need a referral for additional assessment as they don’t disappear spontaneously. Incarceration or strangulation rarely occurs with epigastric hernias.
Inguinal hernias
If a child presents with an inguinal hernia in the first few months of life, there’s an increased risk of strangulation, and surgical repair should be undertaken quickly. The risk drops after one year of age, and the parents may opt to have the surgery done electively. Asymptomatic inguinal hernias in older children should also be referred, despite the risk of incarceration decreasing with age.
In the emergency department, we can attempt to reduce the hernia unless the overlying skin is erythematous. This implies that some ischaemia has already occurred. Try to keep the child comfortable until the surgical team can see them. Reducible hernias may be left for a 12-24-hour waiting period to allow oedema to settle before surgical repair. If the hernia is irreducible, then an urgent operation is needed. In girls, a torted ovary that has passed through the patent processus vaginalis will require urgent surgical repair to save the ovary.
Concerningly, 15% of reduced incarcerated inguinal hernias will re-incarcerate within 5 days if not repaired, so it is important to discuss this risk with the patient or their parents.
Have you heard of the six/two rule for the surgical correction of inguinal hernias?

Neonates tend to be repaired before discharge. In a child under six months, repair should take place on the next available date. Older children may opt for elective day case repairs.
Femoral hernias
Need to be treated ASAP due to the risk of strangulation.
Selected References
Al-Shanafey S, Giacomantonio M. Femoral hernia in children. J Paediatr Surg. 1999;34(7):1104-1106. Available from: https://pubmed.ncbi.nlm.nih.gov/10442600/
Bowling K, Hart N, Cox P, Srinivas G. Management of paediatric hernia. BMJ. 2017;359:j4484. Available from: https://pubmed.ncbi.nlm.nih.gov/29051195/
Hernia. Great Ormond Street Hospital for Children. Available from: https://www.gosh.nhs.uk/conditions-and-treatments/conditions-we-treat/hernia/
Inguinal Hernia in Infants & Children. American Academy of Paediatrics. 2019. Available from: https://www.healthychildren.org/English/health-issues/conditions/abdominal/Pages/Inguinal-Hernia.aspx#:~:text=Hernias%20can%20occur%20at%20any,child%20is%20straining%20or%20crying.
Wu C. Saving Balls 101: The Acute Scrotum. Don’t Forget the Bubbles. 2014. Available from: https://dontforgetthebubbles.com/saving-balls-101-inguinoscrotal-masses/